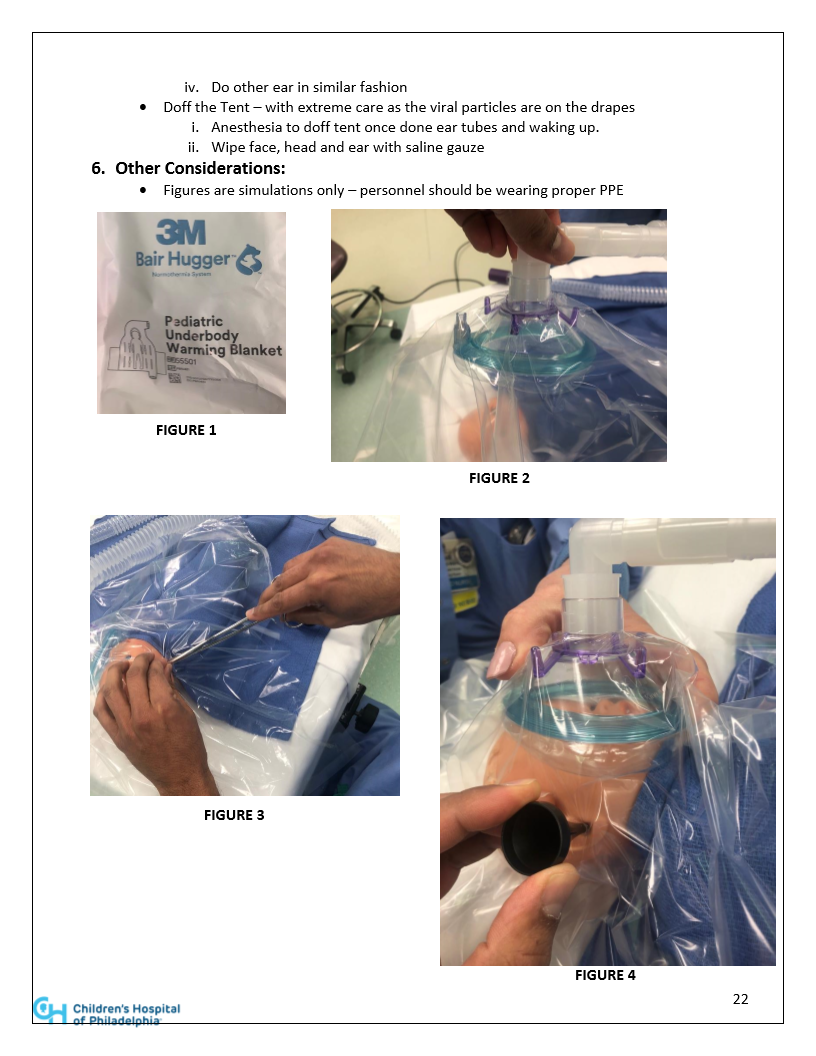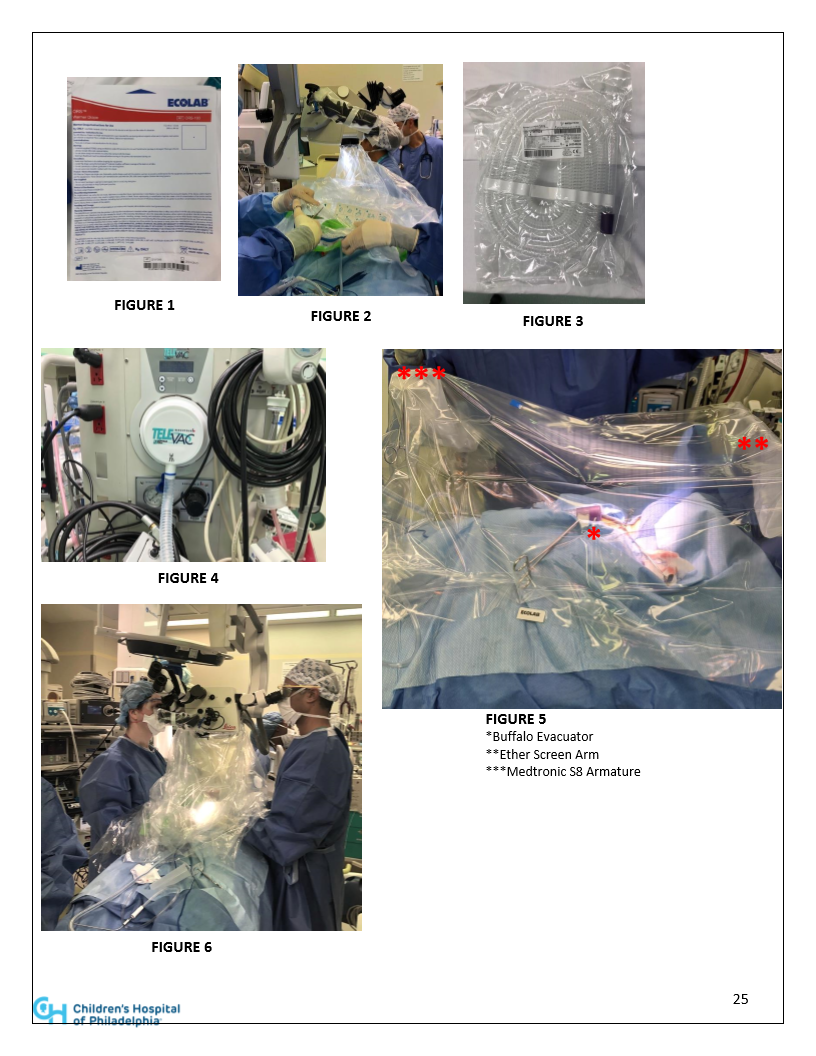
Pearls for Pre-op COVID testing
- Find out who the APP in charge of the RRC is the day you are going to meet patients,
and tiger text that individual the day before.
- Go to the lobby at 7:20 and have the APP in charge text you when the patient(s) is/are checking in.
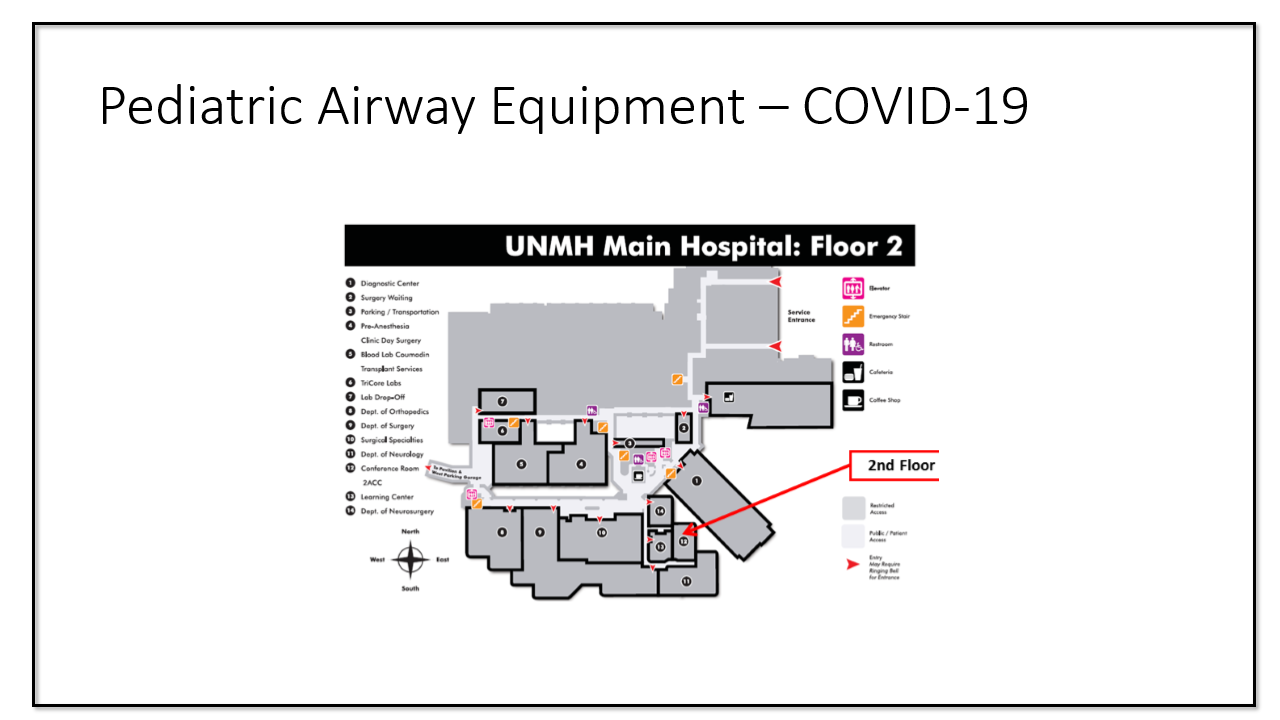
- Patients will go into the RRC through an outside entrance, you
will go in through the BBRP lobby entrance (right next to the elevators). My badge didn't work, but they let me
in because I had coordinated with them. SEE PIC BELOW.
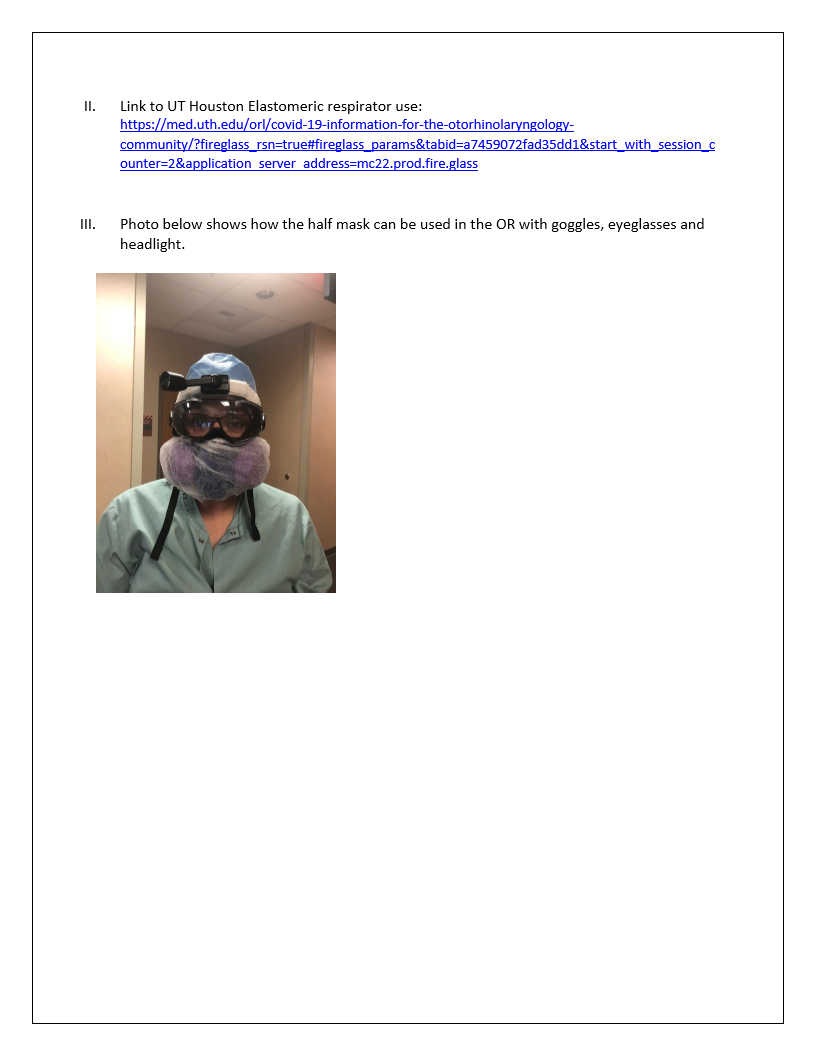
- BRING YOUR OWN N95 and EYE SHIELD. They have gloves and buffonts and overmask and yellow smocks for you. SEE PIC
- Once the patient is ready for testing and you're all PPE'd up, collect the test. Stick the swab all
the way into the nasopharynx. There's a red line on the swab to indicate the depth. Twirl the swab for a
few seconds to saturate it.
- Doff your PPE, send off a quick email to prioritize the test if needed (SEE PIC), and you're done!!!

The staff entrance to the RRC
|

Where you put the rest of your PPE on. Just inside the door.
|
Shoot off a quick email...
|
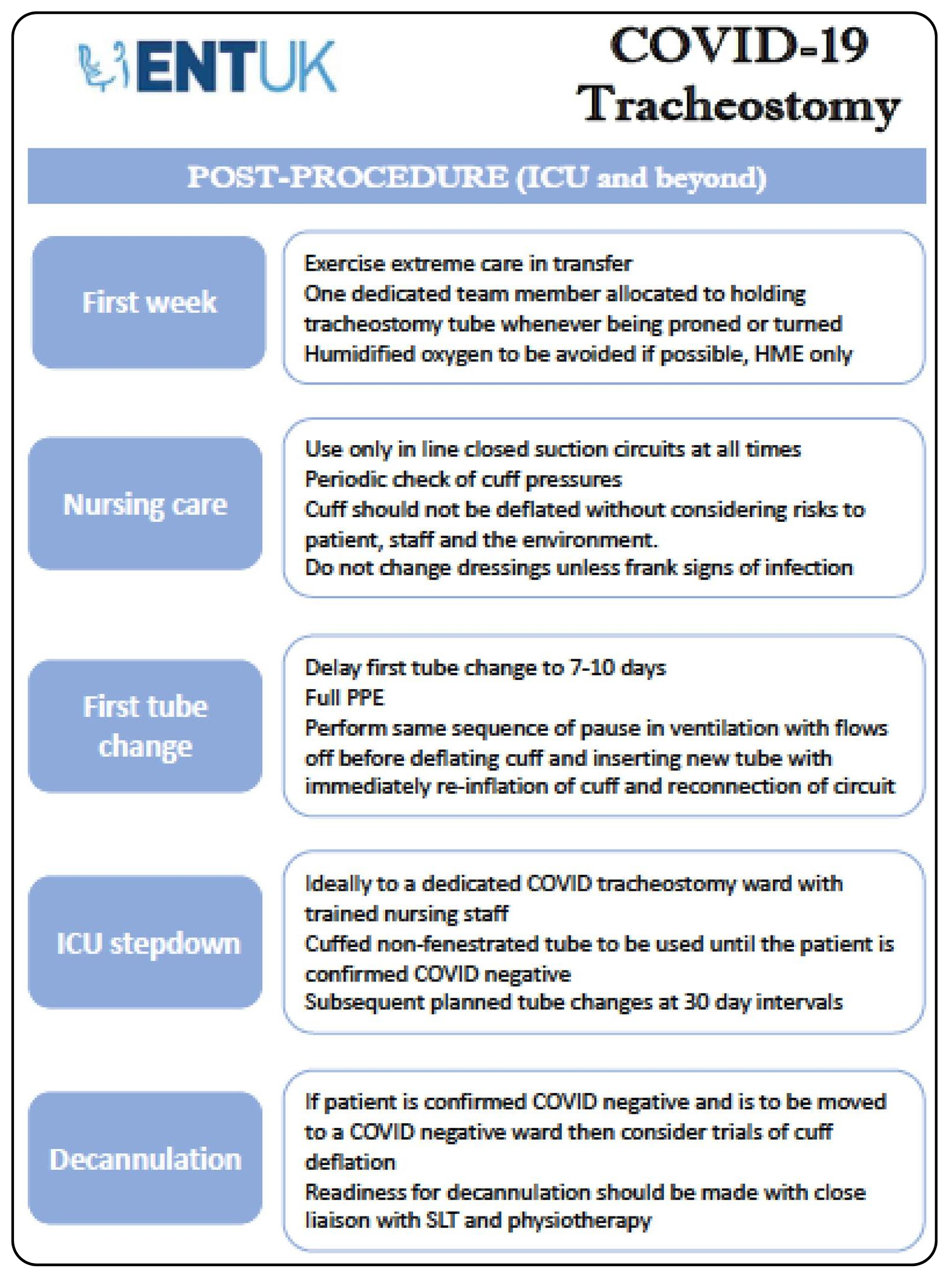
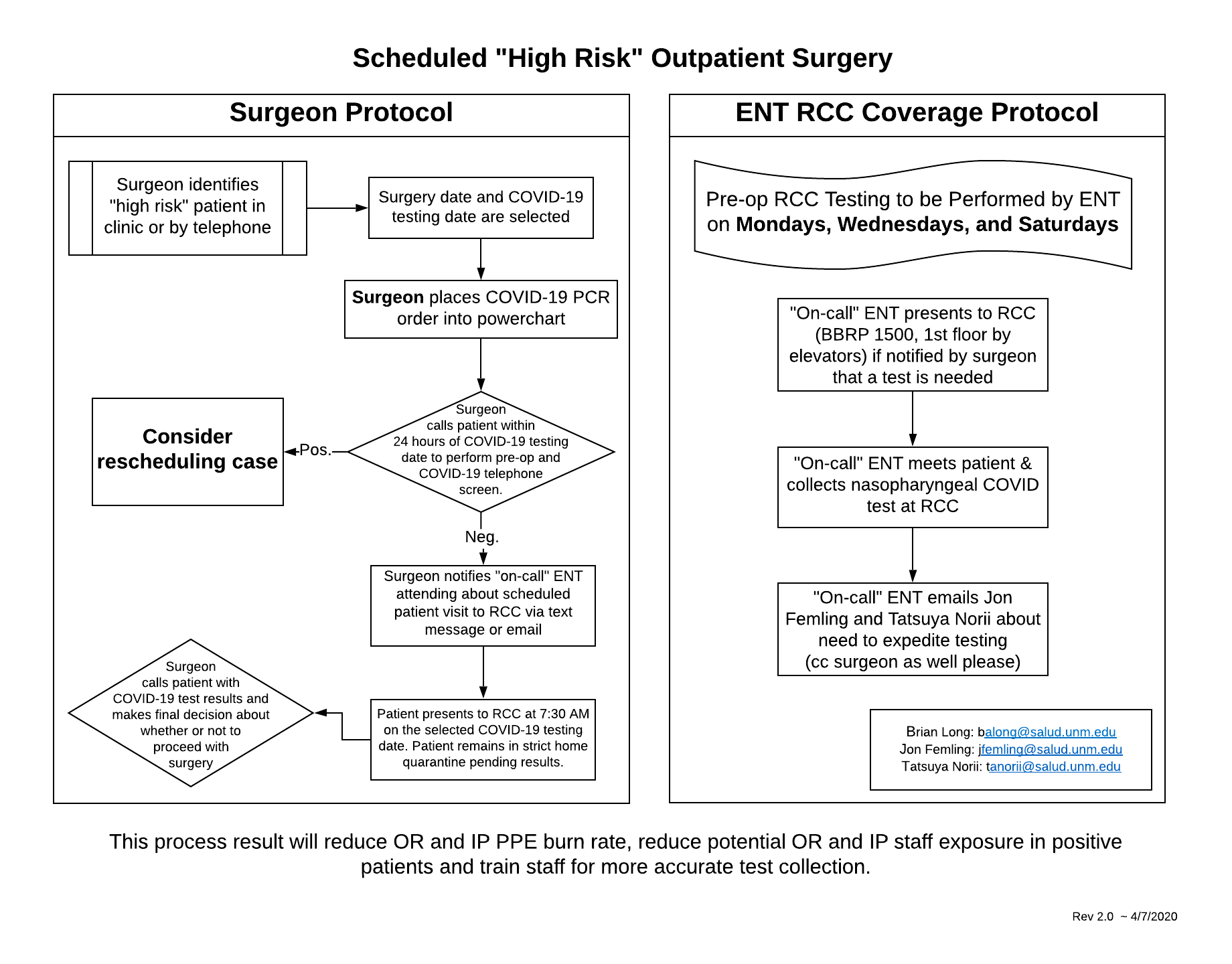
Pre-Operative COVID-19 Testing Protocol
- Non-emergent/urgent aerosolizing procedures will be avoided whenever possible.
- When possible, it is recommended to obtain pre-operative testing for COVID-19 in the setting of aerosolizing procedures. This aims to minimize the overuse of PPE and protect healthcare workers from COVID-19.
If an aerosolizing procedure is unavoidable and pre-operative testing can be performed, the following protocol should be followed:
- Patients requiring pre-operative testing for COVID-19 will be selected by the surgeon.
- A negative test should be obtained within 48-72 hours of the patient’s procedure.
- A patient with a positive COVID-19 result should be treated/quarantined appropriately and, if possible, surgery delayed until viral shedding has ceased
- If an aerosolizing procedure is required and the asymptomatic patient tests negative, the surgeon can elect to downgrade PPE; ie use N95 rather than CAPR/PAPR
- If a patient has a positive screen for COVID-19 and a negative test, the surgeon must discuss with anesthesia team and decide if they'd need to proceed with caution
- ALL pre-operative testing for asymptomatic patients will be performed BY THE SURGEON. PPE to be worn during testing includes: surgical mask, face shield/eye protection and gloves. N95 was not felt to be needed and an overuse use of N95s
OUTPATIENTS:
- At least 3 days prior to the scheduled procedure, the patient will be called by the surgeon to assess patient readiness; Is the case still appropriate? Does the case need to be cancelled for any reason? Ie; illness, inadequate pre-operative medical optimization, etc.
- Pre-operative COVID-19 testing will occur at the RRC
- This location is staffed 24 hours/day and complies with all CDC COVID-19 testing recommendations
- If testing is felt to be appropriate, the patient will be directed where to go and needs to arrive at the RCC at 7:30am.
- The staff Attending/APP for the RCC (found on Amion under "ED Attending;" subcategory "Respiratory Screening") will be notified this patient will be coming in.
- The actual ordering of the test in the RCC will be by surgeon or RCC staff; please communicate follow up plan for results.
- The surgeon will reassess readiness for surgery and screen for COVID symptoms. If appropriate, he/she will collect the sample and walk it to the lab.
- Jon Femling (jfemling@salud.unm.edu) and Tatsuya Norii (tanorii@salud.unm.edu) MUST be notified of the test in order to prioritize the results.
- The patient needs to adhere to quarantine instructions at home while awaiting results.
- The patient will not enter the hospital for surgery until their COVID-19 status is known.
INPATIENTS:
- The ordering provider for the test will be the attending surgeon; order can be placed now with "clinical judgement" as an indication.
- Nasopharyngeal swab must be obtained per hospital protocol and specimen to be walked over the lab, cannot use the tubing system.
- The patient’s COVID-19 testing should be performed with the shortest turn-around time to expedite use of the operative rooms (request for 24-48 turn-around is acceptable)
- Jon Femling (jfemling@salud.unm.edu) MUST be notified of the test in order to prioritize the results.
- The surgeon is responsible for obtaining COVID-19 results and communicating with the primary team (if not the surgical team), anesthesia and the operating room teams the results and further surgical plans for the patient
- The patient does not leave their hospital room until COVID-19 status has been confirmed, they must adhere to strict quarantine while test is pending (patient should wear a mask, wash hands often).